|
PS25 -Improving Health Outcomes of Older Adults by Family Medicine Residency Coordination with a Local Social Service Agency
Video Link
Poster Presenter:
Andrew Collins, Deaconess Family Medicine Residency, Evansville, IN
Objectives:
Identify the most at risk geriatric populations (>60) and increase access to adjunct geriatric services in their area through coordination with their primary care provider.
Methods:
Through use of screening questionnaire, resident PCPs identified patients based on risk for not having food/medications, social support and/or proper shelter. Patients who demonstrated moderate to major concern were then contacted by PCP and then referred to a dedicated SWIRCA case manager.
Upon Referral, SWIRCA utilizes a screening instrument that assesses things such as advanced care planning, adequate supplies of medication and toiletries, access to regular meals, and regular activity. Referral resources and/or actions were then allocated once need identified.
Results:
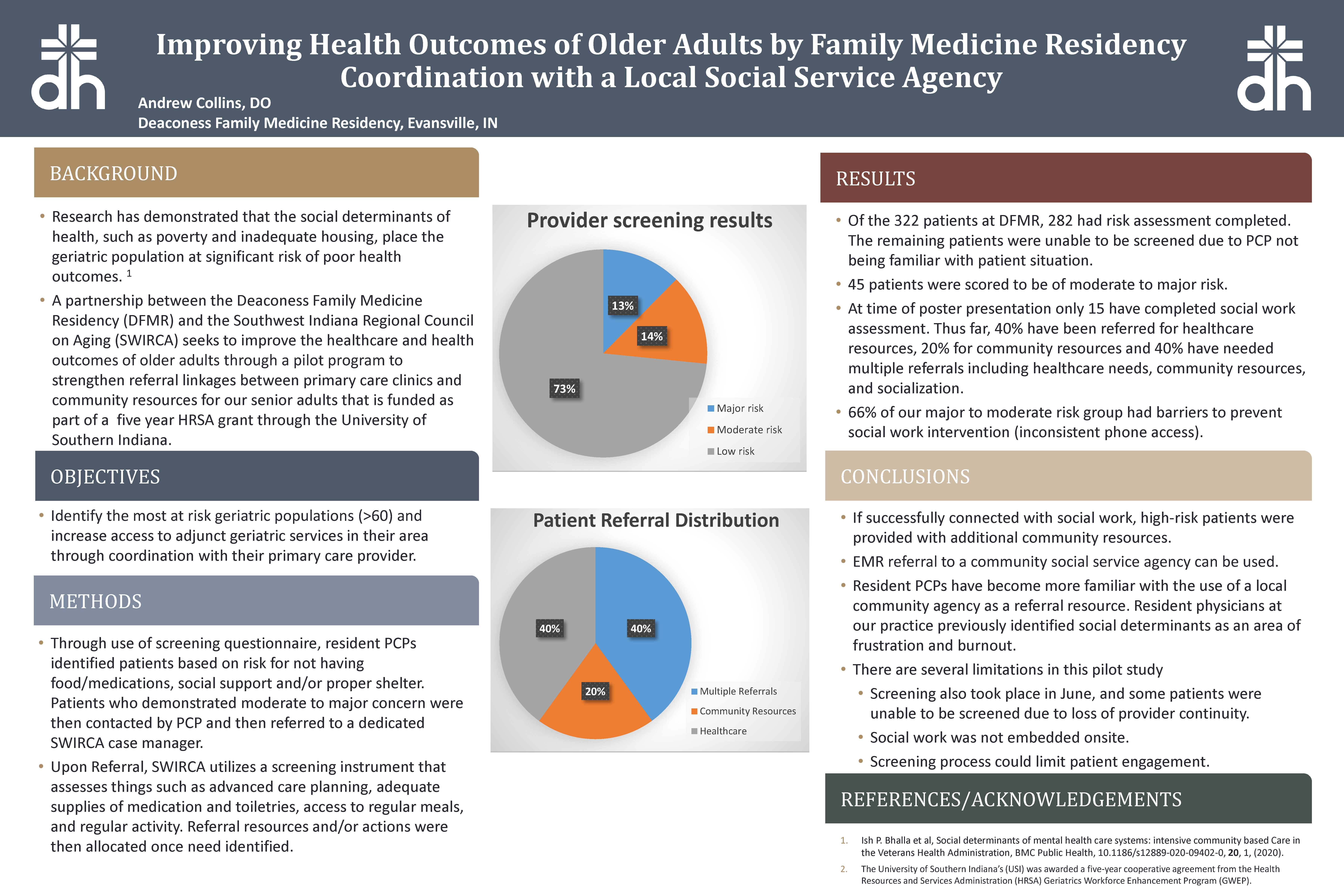
Of the 322 patients at DFMR, 282 had risk assessment completed. The remaining patients were unable to be screened due to PCP not being familiar with patient situation.
45 patients were scored to be of moderate to major risk.
At time of poster presentation only 15 have completed social work assessment. Thus far, 40% have been referred for healthcare resources, 20% for community resources and 40% have needed multiple referrals including healthcare needs, community resources, and socialization.
66% of our major to moderate risk group had barriers to prevent social work intervention (inconsistent phone access).
Conclusions:
If successfully connected with social work, high-risk patients were provided with additional community resources.
EMR referral to a community social service agency can be used.
Resident PCPs have become more familiar with the use of a local community agency as a referral resource. Resident physicians at our practice previously identified social determinants as an area of frustration and burnout.
There are several limitations in this pilot study
Screening also took place in June, and some patients were unable to be screened due to loss of provider continuity.
Social work was not embedded onsite.
Screening process could limit patient engagement.
|